Today is our second episode in our collaborative series with BMJ Thorax. Our mission at Pulm PEEPs is to disseminate and promote pulmonary and critical care education, and we highly value the importance of peer reviewed journals in this endeavor. Each month in BMJ Thorax, a journal club is published looking at high yield and impactful publications in pulmonary medicine. We will be putting out quarterly episodes in association with Thorax to discuss a journal club publication and synthesize four valuable papers. This week’s episode covers four articles related to lung health, COPD, and emphysema.


Meet Our Guests
Chris Turnbull is an Associate Editor for Education at Thorax. He is an Honorary Researcher and Respiratory Medicine Consultant at Oxford University Hospitals. In addition to his role as Associate Editor for Education at BMJ Thorax, he is also a prominent researcher in sleep-related breathing disorders.
Ewan Mackay is a Respiratory Clinical Research Fellow who has started his PhD in London. His research focus is on chronic cough and in the development of new patient-reported outcome measures as well as respiratory physiology, particularly in relation to exercise and disease.
Journal Club Papers
- Journal club article from Thorax
- Estimated health effects from domestic use of gaseous fuels for cooking and heating in high-income, middle-income, and low-income countries: a systematic review and meta-analyses
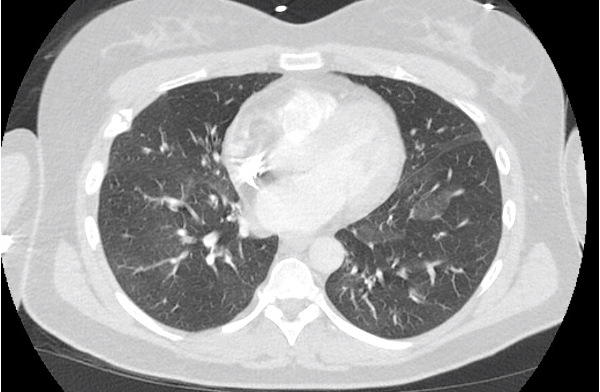
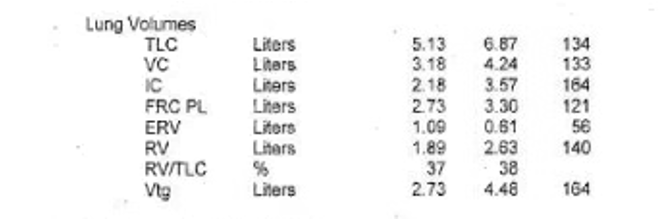
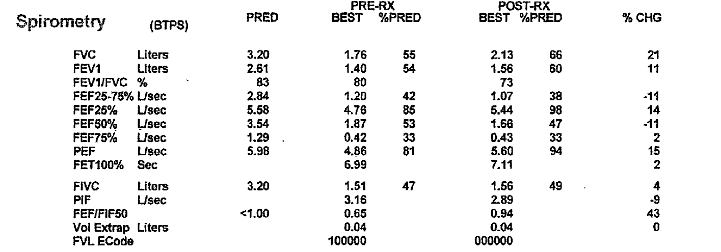
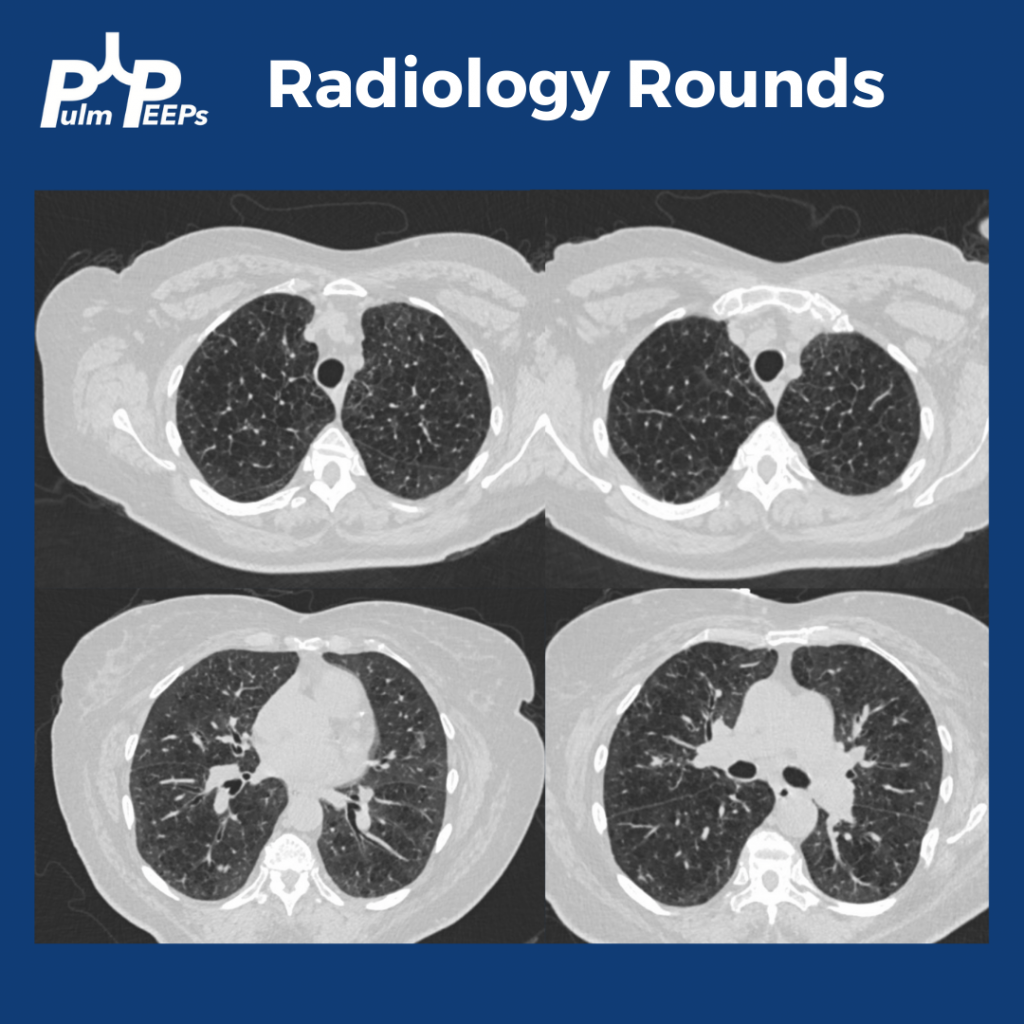
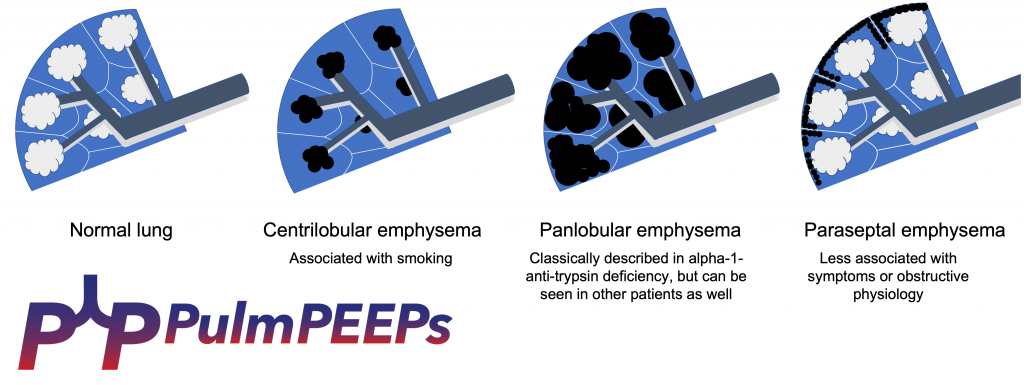
- Structural Predictors of Lung Function Decline in Young Smokers with Normal Spirometry
- Association of Ground-Glass Opacities with Systemic Inflammation and Progression of Emphysema
- Inhaled treprostinil in pulmonary hypertension associated with COPD: PERFECT study results
To submit a journal club article of your own to Thorax, you can contact Chris directly – christopher.turnbull@ouh.nhs.uk
To engage with Thorax, please use the social media channels (Twitter – @ThoraxBMJ; Facebook – Thorax.BMJ) and subscribe on your preferred platform, to get the latest episodes directly on your device each month.
Podcast: Play in new window | Download
Subscribe: Apple Podcasts | Spotify | Amazon Music | Android | iHeartRadio | Podcast Index | RSS