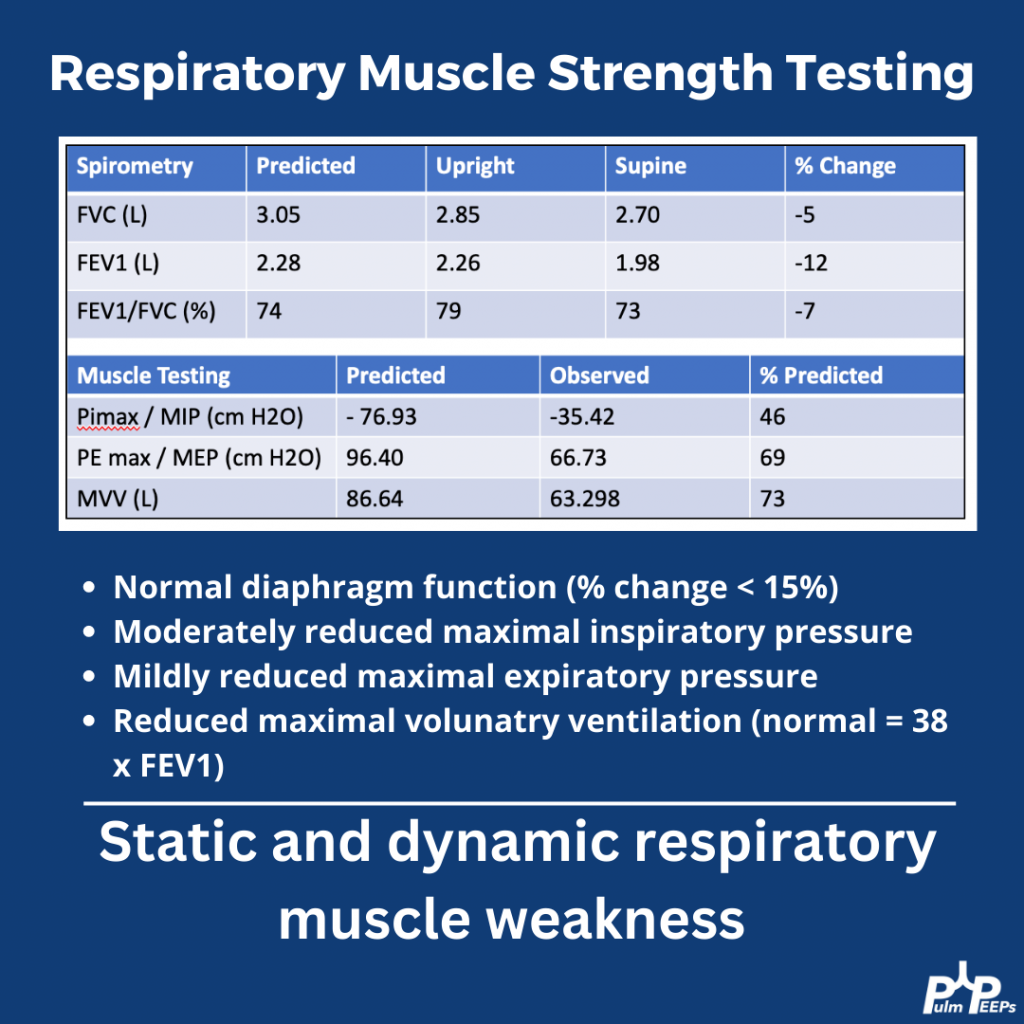
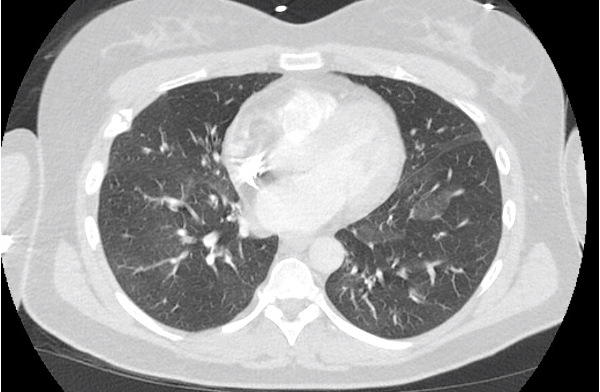
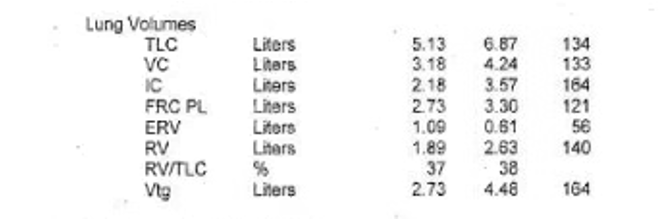
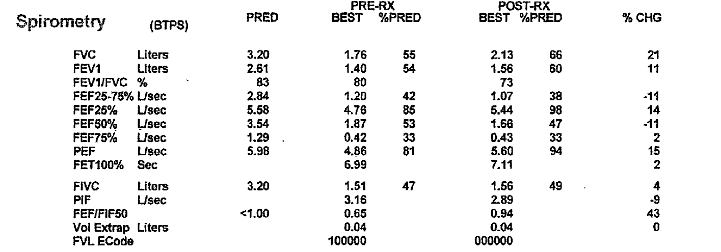
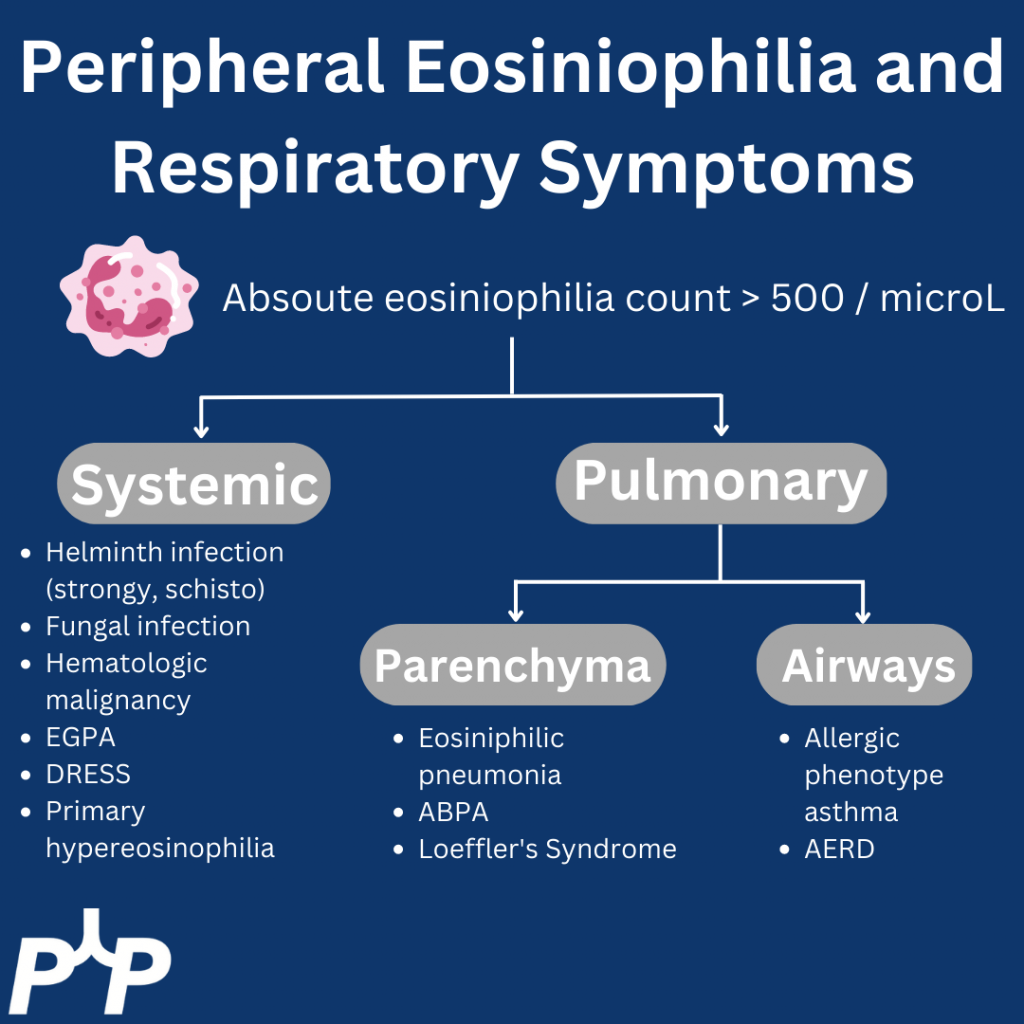
We are excited to bring you a fantastic episode today where we are joined by two guest experts to discuss the recent JAMA Surgery manuscript, “Clinical Implications of Removing Race-Corrected Pulmonary Function Tests for African American Patients Requiring Surgery for Lung Cancer“

Meet our Guests
Sidra Bonner is a general surgery resident at Michigan Medicine. She completed her undergraduate education at Cornell University and medical education at the University of California-San Francisco. Sidra also has a Master’s in Public Health focused in Health Policy from Harvard and a Master’s in Science Health and Healthcare Research from the University of Michigan. She is interested in pursuing a career in general thoracic surgery with a research focus aimed at addressing the multi-level contributors to racial and ethnic inequities in access, quality, and outcomes of surgical care for patients with lung and esophageal cancer.
Tom Valley is an Associate Professor in the Division of Pulmonary and Critical Care Medicine at the University of Michigan. He completed his IM residency and chief residency at the University of Texas-Southwestern/Parkland Memorial Hospital and then joined the University of Michigan as a pulmonary and critical care fellow in 2013 and stayed on for faculty and is the physician-lead for the University of Michigan Schwartz Rounds for Compassionate Care. Tom’s research aims to understand and improve medical decision making in the intensive care unit.
Podcast: Play in new window | Download
Subscribe: Apple Podcasts | Spotify | Amazon Music | Android | iHeartRadio | Podcast Index | RSS