Luke Hedrick, Dave Furfaro, and recurrent RFJC guest Robert Wharton are joined again today by Nicole Ng to discuss the FIBRONEER-IPF trial investigating Nerandomilast in patients with IPF. This trial was published in NEJM in 2025 and looked at Neradomilast vs placebo for treating patients with IPF, on or off background anti-fibrotic therapy. This agents is now FDA approved for pulmonary fibrosis, and understanding the trial results is essential for any pulmonary physician treating patients with IPF or progressive pulmonary fibrosis.

Article and Reference
Today’s episode discusses the FIBRONEER-IPF trial published in NEJM in 2025.
https://www.nejm.org/doi/abs/10.1056/NEJMoa2414108
Meet Our Guests
Luke Hedrick is an Associate Editor at Pulm PEEPs and runs the Rapid Fire Journal Club Series. He is a senior PCCM fellow at Emory, and will be starting as a pulmonary attending at Duke University next year.
Robert Wharton is a recurring guest on Pulm PEEPs as a part of our Rapid Fire Journal Club Series. He completed his internal medicine residency at Mt. Sinai in New York City, and is currently a pulmonary and critical care fellow at Johns Hopkins.
Dr. Nicole Ng is an Assistant Profess of Medicine at Mount Sinai Hospital, and is the Associate Director of the Interstitial Lung Disease Program for the Mount Sinai National Jewish Health Respiratory Institute.
Infographic

Key Learning Points
Why this trial mattered
- IPF therapies remain limited: nintedanib and pirfenidone slow (but do not stop) decline and often cause GI side effects.
- Nerandomilast is a newer agent (a preferential PDE4B inhibitor) with antifibrotic + immunomodulatory effects.
- Phase 2 data (NEJM 2022) looked very promising (suggesting near-“halt” of FVC decline), so this phase 3 trial was a big test of that signal.
Trial design essentials
- Industry-sponsored, randomized, double-blind, placebo-controlled, large multinational study (332 sites, 36 countries).
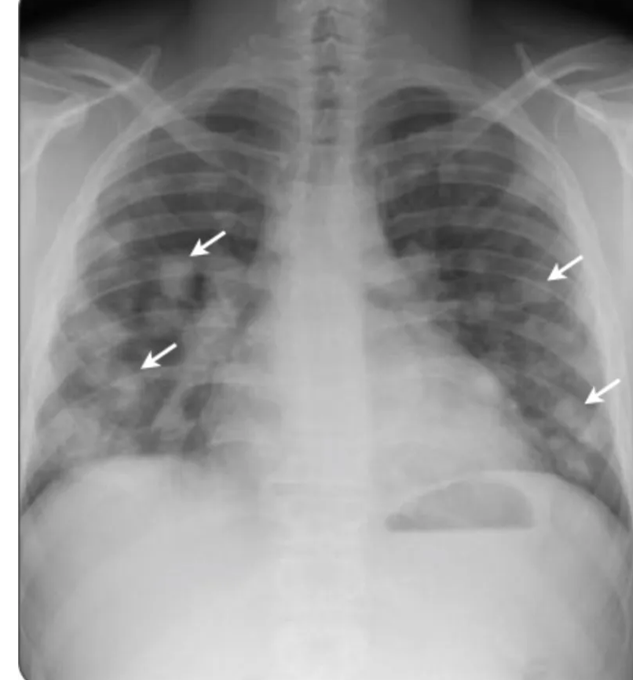
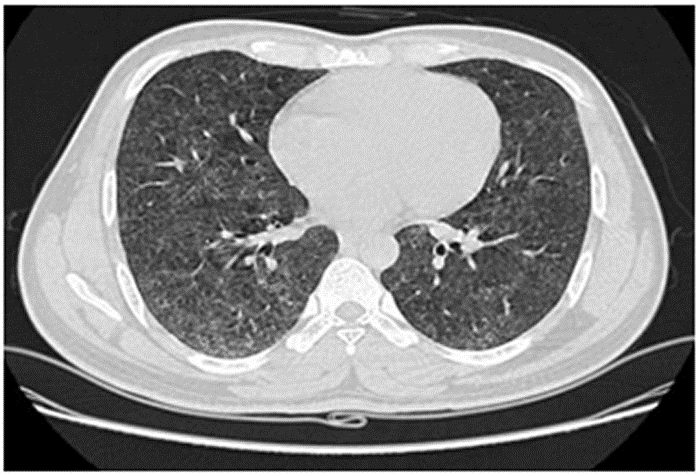
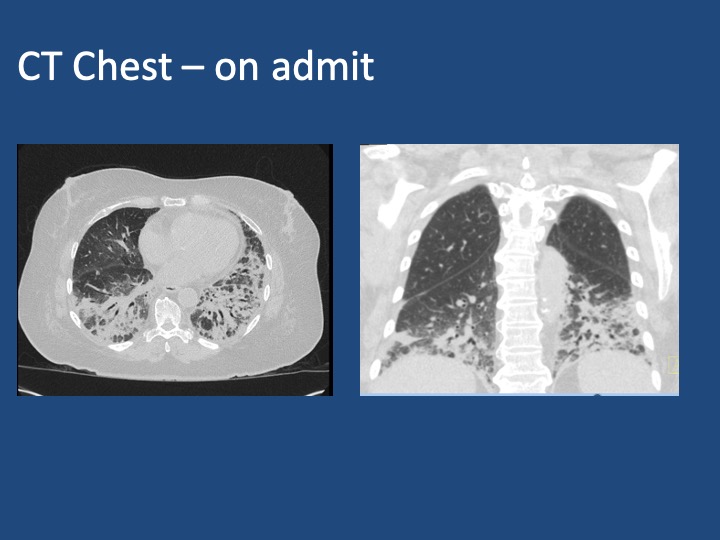
- Population: IPF diagnosed via guideline-aligned criteria with central imaging review and multidisciplinary diagnostic confirmation.
- Intervention: nerandomilast 18 mg BID, 9 mg BID, or placebo; stratified by background antifibrotic use.
- Primary endpoint: change in FVC at 52 weeks, analyzed with a mixed model for repeated measures.
- Key secondary endpoint: time to first acute exacerbation, respiratory hospitalization, or death (composite).
Who was enrolled
- Typical IPF trial demographics: ~80% male, mean age ~70, many former smokers.
- Many were already on background therapy (~45% nintedanib, ~30–33% pirfenidone).
- Notable exclusions included significant liver disease, advanced CKD, recent major cardiovascular events, and psychiatric risk (suicidality/severe depression), reflecting class concerns seen with other PDE4 inhibitors.
Efficacy: what the primary endpoint showed
- Nerandomilast produced a statistically significant but modest reduction in annual FVC decline vs placebo (roughly 60–70 mL difference).
- Importantly, it did not halt FVC decline the way the phase 2 data suggested; patients still progressed.
Important nuance: interaction with pirfenidone
- Patients on pirfenidone had ~50% lower nerandomilast trough levels.
- Clinically: 9 mg BID looked ineffective with pirfenidone, so 18 mg BID is needed if used together.
- In those not on background therapy or on nintedanib, 9 mg and 18 mg looked similar—suggesting the apparent “dose-response” might be partly driven by the pirfenidone drug interaction
Secondary and patient-centered outcomes were neutral
- No demonstrated benefit in the composite outcome (exacerbation/resp hospitalization/death) or its components.
- Quality of life measures were neutral and declined in all groups, emphasizing that slowing FVC alone may not translate into felt improvement without a disease-reversing therapy.
- The discussants noted this may reflect limited power/duration for these outcomes and mentioned signals from other datasets/pooling that might suggest mortality benefit—but in this specific trial, the key secondary endpoint was not positive.
Safety and tolerability
- Diarrhea was the main adverse event:
- Higher overall with the 18 mg dose, and highest when combined with nintedanib (up to ~62%).
- Mostly mild/manageable; discontinuation due to diarrhea was relatively uncommon (but higher in those on nintedanib).
- Reassuringly, there was no signal for increased depression/suicidality/vasculitis despite psychiatric exclusions and theoretical class risk.
How to interpret “modest FVC benefit” clinically
- The group framed nerandomilast as another tool that adds incremental slowing of progression.
- They emphasized that comparing absolute FVC differences across trials (ASCEND/INPULSIS vs this trial) is tricky because populations and “natural history” in placebo arms have changed over time (earlier diagnosis, improved supportive care, etc.).
- They highlighted channeling bias: patients already on antifibrotics may be sicker (longer disease duration, lower PFTs, more oxygen), complicating subgroup comparisons.
Practical takeaways for real-world use
- All three antifibrotics are “fair game”; choice should be shared decision-making based on goals, tolerability, dosing preferences, and logistics.
- Reasons they favored nerandomilast in practice:
- No routine lab monitoring (major convenience advantage vs traditional antifibrotics).
- Generally better GI tolerability than nintedanib.
- BID dosing (vs pirfenidone TID).
- Approach to combination therapy:
- They generally favor add-on rather than immediate combination to reduce confusion about side effects—while acknowledging it may slow reaching “maximal therapy.”
- Dosing guidance emphasized:
- Start 18 mg BID for IPF, especially if combined with pirfenidone (since dose reduction may make it ineffective).
- 9 mg BID may be considered if dose reduction is needed and the patient is not on pirfenidone (e.g., monotherapy or with nintedanib).
Podcast: Play in new window | Download
Subscribe: Apple Podcasts | Spotify | Amazon Music | Android | iHeartRadio | Podcast Index | RSS